
Financial Burden in U.S. Healthcare is not a recent topic of discussion. Beyond inflation, the clinical practice business has become increasingly complex because of staffing, medical advances, the addition of new treatments, incorporation of electronic health data, new regulations, pandemic response and growing patient demand for services.
The pandemic alone left lasting emotional and financial effects on hospitals and health systems. After the COVID-19 pandemic caused expenses to increase as health systems experienced declines in patient volumes for non-emergent care but surges in COVID-19 hospitalizations that required complex care.
Even if 2023 is expected to be the start of slow economic recovery from the pandemic, healthcare providers are also faced with growing administrative burdens, such as prior authorization requirements and disputing health insurers post‐hoc denials of those approvals, which demand an exorbitant amount of time and resources to process resulting in one third of patients reporting a billing problem or prior authorization requirement delayed or even missed care.
The combination of decreased physician reimbursements from the Centers for Medicare & Medicaid Services and insurance companies as well as increased procedure costs, continues —now more than ever— to put physician pay in danger.
“What we’re seeing with that is decreased reimbursement rates, especially in our rural communities, decreases their financial viability and they may have to close doors,” says Angela Mund, President of the American Association of Nurse Anesthesiology (AANA).
Physician payment is always in the crosshairs and the one that is sacrificed while insurance companies continue to create greater healthcare costs every year by driving providers to navigate more complicated administrative challenges. This only drains revenue from the communities they serve starting with Rural zones, and physicians especially in remote areas will not be able to sustain continual cuts to their reimbursement.
“Recently, a major insurance company in the United States implemented a national policy to decrease CRNA reimbursement by 15%. This 15% cut, when hospitals are potentially already struggling to survive,” added Tracy Paul Young, Regional Director, AANA and CEO, YPS Anesthesia
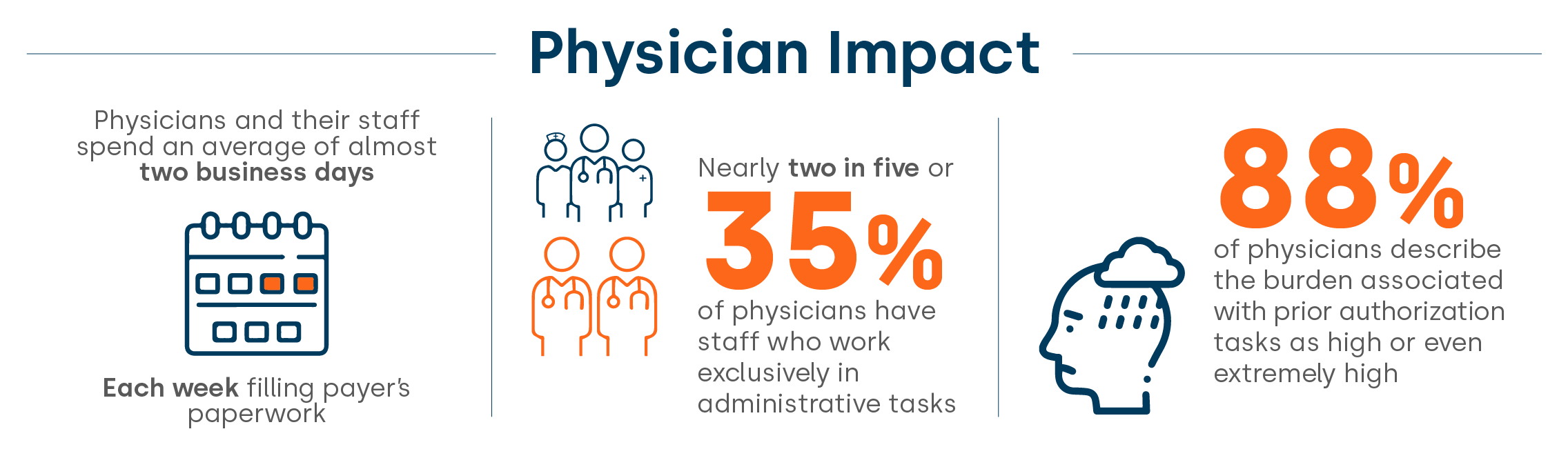
What happens in the Rural Setting?
As a result, Rural based physicians are faced with harsh realities. Do they sell their practice to a hospital? Do they cut their losses and retire early? Do they stop seeing patients at rural facilities and limit their practice to urban locations? Should they stay away expensive new treatment options and modern devices that could provide better care? Should they operate with minimum staff? All these considerations impact patients’ access to quality healthcare and health equity, especially for the underserved population.
Low accessibility, poor and rural communities deserve affordable, accessible, and quality healthcare. With over 14 years of experience in Medical Billing and Revenue Cycle Management, Smrtdo helps Rural healthcare providers reduce revenue cycle complexity, freeing your staff from administrative challenges so you can focus on improving quality and delivering care in their communities. Our services and expertise help streamline the operation side of your practice, diagnose performance gaps, achieve the highest coding accuracy, resolve difficult accounts receivable and implement patient-centered solutions to your current pain points.
In the last 4 years we have helped over 9 Rural Hospitals in the United States to avoid bankruptcy while reducing their financial vulnerability and we can deliver the same results for you!
Our experts will take care of your medical billing and collection, so you can focus on your patients.
Quick Links
Follow Us
© Copyright 2019 Smrtdo Medical Billing All Rights Reserved, Designed by Hite Digital | Privacy Policy | Terms & Conditions

